Disordered Eating & Dieting
Disordered eating sits on a spectrum between normal eating and an eating disorder and may include symptoms and behaviours of eating disorders, but at a lesser frequency or lower level of severity. Disordered eating may include restrictive eating, compulsive eating, or irregular or inflexible eating patterns. Dieting is one of the most common forms of disordered eating.
Other behaviours that may be present in a person engaging in disordered eating include:
• Fasting
• Binge eating
• Skipping meals
• Avoiding a type of food or food group
• Self-induced vomiting
• Laxative, diuretic, enema misuse
• Steroid and creatine use
• Using diet pills
Australian adolescents engaging in dieting are five times more likely to develop an eating disorder than those who do not diet (1).
Why are disordered eating and dieting so dangerous?
Disordered eating behaviours and in particular dieting are among the most common risk factors for the development of an eating disorder. Eating disorders are severe and life-threatening mental illnesses. An eating disorder is not a lifestyle choice.
Restricting the amount of food you eat can result in a series pf changes in the body. When the body is starved of food it responds by reducing the rate at which it burns energy (the metabolic rate) and this can result in over eating and binge eating behaviours. Dieting is also associated with other mental health concerns including depression and anxiety.
Disordered eating can have a negative impact on a person’s life and has been linked to a reduced ability to cope with stressful situations. Feelings of guilt, shame and failure are common in people who engage in disordered eating. These feelings can arise as a result of binge eating or ‘breaking’ a diet. A person with disordered eating behaviours may isolate themselves for fear of socialising in situations where people will be eating. This can contribute to low self-esteem and social withdrawal.
Dieting and the diet cycle
Dieting is one of the strongest predictors for the development of an eating disorder. Weight loss and ‘fad’ diets do not take people's individual requirements into consideration and can result in a person feeling hungry, experiencing low moods, lacking in energy levels and developing poor mental and physical health.
The ‘diet cycle’ explains how many eating disorders can develop and are maintained.
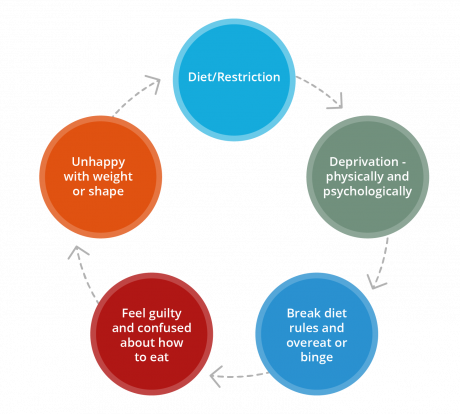
Diet/restriction:
A person limits the amount of food or type of food eaten.
Deprivation:
When food intake is restricted, the body responds both physically and mentally. The metabolism slows down to conserve energy, appetite increases and the craving for the restricted foods increases. At this stage, people may feel deprived, irritable and fatigued.
Break diet rule:
The diet rules are almost inevitably broken, with the body wanting and needing the food that has been restricted. Overeating can often follow.
Feelings:
When breaking the diet rule, people are often left with feelings such as guilt, low self-esteem and negative body image. People may feel that they have failed and that they lack willpower.
Unhappy with weight or shape:
With these feelings comes a resolve to ‘do better’. People are often led back to the diet or restriction, and the diet cycle begins again.
What are the risks associated with disordered eating and dieting?
The risks associated with disordered eating are severe. People with disordered eating may experience:
• A clinical eating disorder such as anorexia nervosa, bulimia nervosa, binge eating disorder or other specified feeding and eating disorders (OSFED)
• Osteoporosis or osteopenia: a reduction in bone density caused by a specific nutritional deficiency
• Fatigue and poor sleep quality
• Gastrointestinal problems such as constipation and/or diarrhoea
• Headaches
• Muscle cramps
• Feelings of shame, guilt, and low self-esteem
• Depressive or anxious symptoms and behaviours
• Nutritional and metabolic problems
Changing dieting and disordered eating behaviours
It is possible to change eating behaviour, even if you have been engaging in disordered eating and dieting for many years. With the right support and treatment, behaviour change is possible.
Getting help
If you or someone you know is engaging in disordered eating or dieting behaviour, consider seeking help. Disordered eating and dieting are key risk factors for the development of an eating disorder and seeking help early is the best preventative measure. Your GP is a good ‘first base’ to seek support.
To find help in your local area go to NEDC Support and Services.
Download the disordered eating and dieting fact sheet here.
References
1. Patton GC, Selzer R, Coffey C, Carlin JB, Wolfe R. Onset of adol escent eating disorders: population based cohort study over 3 years. BMJ.
1999;318(7186):765.

