Stages of Change
The stages of change model can be helpful in understanding how a person living with an eating disorder may be thinking and feeling at different stages of illness and recovery.
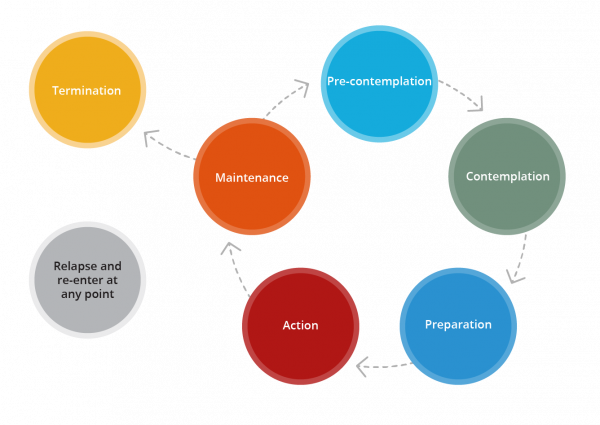
There are six stages of change that a person experiencing an eating disorder may go through. A person may go through this cycle several times or may go back and forth between these stages. The model highlights that while recovery is possible, the course of illness and recovery may not be linear. Throughout each stage there may be behavioural signs which may help you identify what stage the person is in and how you can best approach them.
Stage 1: Pre-Contemplation
In the pre-contemplation stage, a person experiencing an eating disorder may deny that there is a problem. You may have noticed some of the warning signs and feel concerned about the person, but they will have little or no awareness of the problems associated with their eating behaviours. Instead, they may be focused on controlling their eating patterns. In this stage, the perceived benefits (such as using an eating disorder to control or avoid strong emotions) outweigh any costs and the person may not be ready to change and may be afraid to let go of their current coping behaviours. The person may be reluctant to disclose their behaviour and may appear hostile, angry or frustrated when this topic is approached.
What you can do:
• Stay calm and try to see things from their point of view
• Show compassion and understanding
• Take the focus off the eating behaviour. Talk about their interests, goals in life, and the things they may be missing out on as a result of the eating disorder
• Continue to support and hold hope for the person you are supporting
• Become familiar with our tips for talking to someone you are concerned about. You can find these at Tips for Carers.
• Encourage and support access to medical treatment if their health is compromised.
Stage 2: Contemplation
A person experiencing an eating disorder who is within the contemplation stage will have an awareness that something is wrong. They may be considering the benefits of changing some of their behaviours but may be unsure about taking action. As such, the person may experience internal conflict between wanting to change and at the same time wanting to maintain their disordered eating habits. This is sometimes known as ambivalence about recovery. This can be difficult and confusing for both you and the person you are caring for.
What you can do:
• Encourage the person to voice their thoughts, feelings and concerns
• Demonstrate that you are listening to what the person is saying. You can even reinforce what the person is saying by reflecting it back to them (e.g., “I hear you saying that part of you feels like you want to change, while another part of you feels scared of changing...”)
• Show them you respect their ideas, particularly the ones in favour of change
• Gently highlight the discrepancies in their thinking/actions and amplify the positives for change
• Try to boost their self-esteem and confidence. This will help them believe they can change.
Stage 3: Preparation
In this stage, the person experiencing an eating disorder has decided they want to change their behaviour to move away from the eating disorder, and is preparing to make these changes. They usually take small steps to change their behaviour and may begin to engage in conversations about change, and seek support and encouragement to take the next steps. A level of ambivalence about recovery may still be present.
What you can do:
• Be informed. Learn as much as you can about the steps you and the person you are caring for or supporting need to take in order to recover.
• Continue to encourage the person to voice their thoughts, feelings and concerns
• Support the person to access treatment
Stage 4: Action
In the action stage, a person experiencing an eating disorder will be taking steps towards treatment and recovery. They are engaged in treatment and have begun to change the behaviours, thoughts and environment related to the eating disorder. The person will be learning ways and strategies to cope and will be making progress to return to normal eating behaviours. A level of ambivalence about recovery may still be present.
What you can do:
• Acknowledge that it is challenging to change and recover from an eating disorder
• Support the person through challenges and let them know you care for them and believe in them. This will help build their confidence.
Stage 5: Maintenance
In the maintenance stage, a person experiencing an eating disorder will have changed their behaviours and will be proactively implementing new behaviours into everyday life. Eating disorder thoughts and feelings may be reducing in frequency and intensity. The person is working to sustain the new behaviours and navigate the pathway to ongoing recovery. Relapse or a recurrence of eating disorder behaviours and cognitions may occur at this stage. While relapse can be stressful, it is normal and allows the person to develop insight and develop ongoing strategies for recovery.
What you can do:
• Work together with the person to identify triggers that may impact their recovery
• Accept relapse as a part of learning and the process of recovery
• Help them to put systems and strategies in place to help avoid relapse
• Show care, patience and compassion
Stage 6: Termination
Termination is the final stage of the stages of change model. It describes a sustained period with no return to eating disorder behaviours and/or cognitions. During this stage, no matter what situation the person may face, they are confident they will continue to cope in adaptive ways and will not return to disordered eating behaviours or patterns. Ideally, their adaptive behaviours have become largely automatic.
Although full recovery is possible for many people, it is important to recognise that for some a more realistic expectation is ongoing management of eating disorder behaviours, thoughts and feelings.

